By Dr. Bonnie Sawatzky on March 27, 2025
Early in my academic career, my goal was to teach basic research skills like ethics, consenting and data collection and analysis. Students learning from patient participants was minimal.
By Dr. Ras Mulinta on January 23, 2025
For years, I struggled to give feedback that truly supported growth. At times, I masked my own cognitive fatigue, imposter syndrome included, to keep the energy up.
By Dr. Meera Anand on March 18, 2024
Author Dr. Meera Anand (biography and disclosures) Disclosures: The author has nothing to disclose. Disclaimer: The author has nothing to disclaim. What I did before: As a community-based physician, I started my teaching role by taking medical students and residents in my clinic independently and in isolation. I would improve my teaching skills by attending […]
By Dr. Ras Mulinta on January 3, 2024
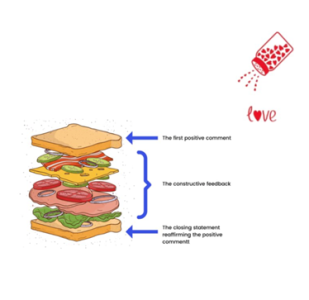
When delivering constructive feedback, I often feared being perceived as insensitive or overly critical, and the sandwich technique often felt insincere, rather than fostering intrinsic motivation.
By Dr. Kelvin Lou on January 1, 2024
How can we approach serious illness conversations? How can we expand and deepen our understanding of existing tools so that we may apply them to situations we don’t anticipate?
By Clarrisa Wallace, Sue Mills and Fahreen Dossa on January 24, 2020
In preparation for teaching a Clinical Skills session, we diligently reviewed the tutor guide and video ahead of time. However, we sometimes wondered how other teachers were translating the advice from the guide into their teaching.
By Lily Zhou on September 4, 2018
I used to feel crushed when looking up from notes during a presentation to a packed lecture hall of colleagues intensely concentrating…
By Michael Lee & Isabeau Iqual on August 8, 2017
Like many teachers, I begin to plan my course by creating course-level learning objectives and after that design the course to meet these.
By Heather Buckley and Nawaaz Nathoo on March 1, 2017
I wondered why new learners just transitioning to new clinical experiences sometimes seemed hesitant to participate and thus appeared less engaged in clinics and journal clubs. I found that some learners would jump in and take part in conversations, discussions, and even engaging with patients.
By Douglas Cave, PhD on August 3, 2015
I was frustrated at times that the students and residents did not always follow the instructions I gave. Their work was sometimes incomplete, off topic, or plainly wrong. While this was not true for most students, it was consistently true for a few each year. Teaching about empathy for example, I would invite residents to practice doing an interview with each other using empathic reflections and they would do it incorrectly.
By Dr. Sue Murphy on July 3, 2015
One of the topics examined in my initial “professionalism” course are the bylaws and Standards of Practice of the licensing body. Bearing in mind that the end goal is that students should be able to apply these standards to practice, not just memorise them, the multiple choice question (MCQ) exam format I have used contained a typical practice scenario with a variety of possible options for action, with instructions for the student to select the “best” option.
By Dr. Deborah Altow on April 1, 2015
Dr. Deborah Altow (biography and disclosures) What I did before Like many teachers, I was seduced by the imperative to make sure my students gained the benefit of my experience, and thus I talked too much. I had always told my students that the two 4-letter words they needed most were KIND and WAIT. One […]
By Dr. Linlea Armstrong on July 4, 2013
Telling our students that “it will be on the exam”, may give us a sense that the students will learn it. This line tends to get used when there is an important topic that the teacher suspects students might otherwise not sufficiently attend to. Yet the strategy is unlikely to inspire deep and long-term learning, the kind of learning that students will later be able to retrieve and apply to patient care.
By Dr. Richard Cohen on January 17, 2013
In the past I followed a tried and tested format for classroom lecturing ‘Tell them what you are going to tell them’ (a set of well-written educational objectives), ‘tell them what you want to tell them’ (no shortage of instructional papers on how to develop a good PowerPoint presentation) and finally ‘tell them what you have told them’ (a concise summary).
By Dr. Kiran Veerapen on December 18, 2012
Before this incident in the emergency room, I had no established teaching practice that focused consciously on checking the veracity of a trainees’ use and understanding of medical terminology. This challenged my assumption that the medical student comprehended such composite terms accurately.
By Sue Murphy on June 1, 2012
An ongoing problem with student supervision in the clinical setting is managing the expectations of Clinical supervisors. Frequently, clinical supervisors are clinicians with many years of experience in their specialty, who have not been practicing at “entry level” for some time.














Recent Comments