By Dr. Ilona Hale on April 22, 2026
Shared decision-making (SDM) tools can help patients better understand the absolute risks and benefits of different testing and treatment options, and allow patients to decide what is right for them. By empowering patients, I can not only provide better care but also reduce environmental impacts and unnecessary burdens on the system.
By Dr. Kerstin Gustafson and Dr. Colleen Dy on February 25, 2026
As care providers, we should be ready to respond to our patients’ midlife concerns with accurate and evidence-based information. This article explores commonly prescribed preparations for managing vasomotor symptoms in menopause.
By Dr. Sarah McCorquodale & Dr. Trevor Corneil on January 28, 2026
Endemic measles has returned to BC and Canada, and in 2025 there were 414 cases reported in BC and 5,392 in Canada (confirmed and probable). As such, measles is now on my differential diagnosis for rash and respiratory illness. I implement appropriate infection control measures in my office to protect other patients and staff.
By Dr. David Wilson & Hilary Cullen on September 24, 2025
Concussions/mTBIs aren’t just sports injuries, but falls, vehicle collisions and violence are also common causes. This article shares the new BC Guideline on concussion/mTBI, which emphasizes early assessment, active recovery and practical tools for primary care.
By Dr. Heather Leitch on July 23, 2025
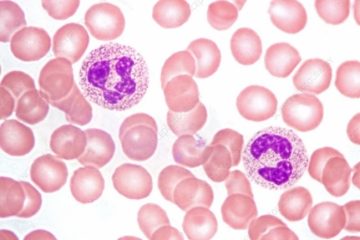
This article provides evidence-based answers to common questions hematologists receive about hemoglobin disorders. Through case examples, I explore best practices for iron repletion and highlight key indicators for when referral to hematology is required.
By Dr. Douglas Green on May 28, 2025
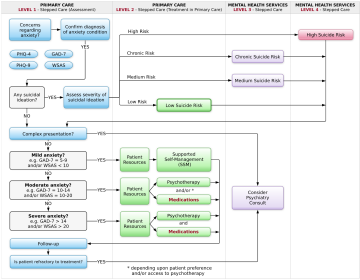
Studies indicate that anxiety conditions are often underdiagnosed and undertreated in primary care. The Ottawa Anxiety Algorithm has been designed to be evidence-based and practical, and contains guidance as to when and how to screen for and diagnose anxiety conditions, self-help resources that can be emailed to patients, links to community resources and treatment algorithms for the commonly used medications for these conditions.
By Dr. Ilona Hale on April 23, 2025
Until recently, I had never really considered that testing and treatments have an environmental cost. The burden of overuse is not trivial: up to 30% of all tests and treatments we order are unnecessary and an additional 10% are harmful to our patients. I have realized that if I really want to make a difference to my carbon footprint at work, reducing unnecessary care has a greater impact than recycling clinic waste or powering down my computer.
By Dr. Kerstin Gustafson and Dr. Colleen Dy on February 26, 2025
Women often seek medical care around the time of menopause, yet, in one survey, only 27% of Canadian women reported that their family physician proactively discussed menopause with them. The root of this care gap is thought to be the paucity of education that medical professionals have received regarding menopause in the last 20 years. Now, we try to include at least one question about menopausal symptoms proactively in our seemingly asymptomatic patients over the age of 40.
By Dr. Judy Dercksen on January 22, 2025
My interactions with high impact chronic pain patients have become more effective as my approach has changed from a relentless pursuit to decrease their pain, to a more compassionate one, where in a safe space I listened as patients shared their needs and goals, while I provided them with tools when they were receptive to change.
By Dr. Heather Fulton on November 26, 2024
I recommend Community Reinforcement and Family Training (CRAFT) for families who have a loved one with substance use challenges. It is a is a science-backed approach that helps family members change the way they interact with their loved one that makes change more likely while also helping themselves in the process.
By Dr. Michelle C. Chan on October 22, 2024
Recent studies on options in family planning have changed my practice, and I now routinely take the opportunity when reviewing family planning options for people who are at risk of becoming pregnant and do not want to be pregnant to review emergency contraception and abortion as options in family planning.
By Dr. Ilona Hale on September 16, 2024
For many years, I failed to recognize the unique potential I had to make a difference to the environment as a clinician, from within my own practice. However, using a planetary health approach in clinical practice not only allows us to reduce environmental impacts but also offers many co-benefits: better health outcomes, lower costs, decreased workload, and a more resilient and sustainable system.
By Dr. Sarah McCorquodale on June 17, 2024
Having evidence that remission of type 2 diabetes is possible through weight loss in select people, I have changed my approach to prevention and management of type 2 diabetes.
By Dr. Omesh Syal on April 15, 2024
I highly recommend registering with the Health Data Coalition and becoming more familiar with your measures within the HDC Discover application to recognize your contribution. We, as a collective profession, can make a positive impact on our own practices and larger communities.
By Dr. Paxton Bach on March 12, 2024
The new Canadian guideline situates alcohol-related harms along a continuum, recognizing that negative health and social consequences of alcohol can arise even at rates previously consistent with low risk.
By Rohit Singla PhD, Dr. Daniel Raff, Dr. Hester Vivier, and Dr. Andre Van Wyk on February 14, 2024
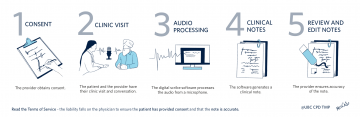
Conversational AI has become a valuable tool for family physicians in Canada. It helps us provide better patient care, eases the burden of documentation, and reduces burnout. Incorporating digital scribe technology brings marked efficiency, especially given the high patient volumes. With AI managing real-time transcription and summarization, physicians can give undivided attention to patients, deepening rapport and focus on prescriptions and referrals.
By Drs. Kevin Liang and Philip Hui on January 10, 2024
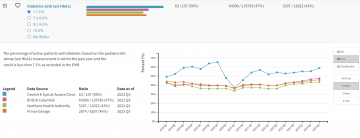
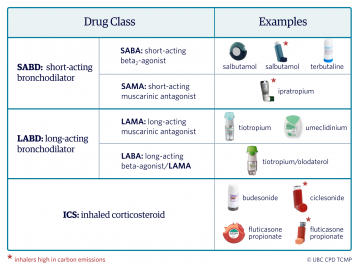
New asthma and COPD guidelines are changing the way we provide respiratory care; SABDs, such as salbutamol and ipratropium, are no longer the mainstay treatment for both conditions. Importantly, SABD overuse is a measure of poor disease control and suggests a need for treatment escalation.
By Dr. Shirley Samuel-Haynes on November 21, 2023
I learned that a palliative approach to care and serious illness conversations address and manage patients’ and families’ psychological, practical, social, loss/grief, spiritual, and physical issues like pain and symptom management in line with their goals of care and help prepare for eventual life closure. Here are practical tips on how to implement this in your practice.
By Dr. Nawaaz Nathoo and Sorayya Seddigh on October 11, 2023
There are currently no eye drops for presbyopia treatment that have been approved for use in Canada. In December 2021, pilocarpine hydrochloride 1.25% eye drops became the first drug approved by the FDA for the medical management of presbyopia. Pilocarpine is a miotic agent that uses the eyes’ natural ability to constrict the pupil via parasympathetic innervation. It has been shown to improve near-intermediate vision without impacting distance vision.
By Drs. Jill Norris and Jessica Otte on September 12, 2023
Primary care clinicians face an overwhelming volume of information to process and tasks to complete. There are new and sometimes conflicting guidelines and practice standards, forms to fill out, emails about meetings, and an inbox full of labs, documents to review, and messages to respond to. Now that I get Portraits in my email inbox from time to time, I schedule time to look at them, and focus on the listed recommendations and whether my pattern of practice is close to where it should be according to the evidence, and if not, why not.
By Drs. Domnick Manhas and Tony Wan on August 23, 2023
It is estimated that 15% of all cancer patients will develop VTE, resulting in significant morbidity and mortality. The cost of cancer-associated thrombosis is substantial to the healthcare system. Currently, routine thromboprophylaxis is not recommended given the fear of increased risk of bleeding, modest absolute risk reduction in VTE, and inconvenience. However, a selected group of cancer patients with very high VTE risk will benefit from thromboprophylaxis.
By Dr. Sander Veldhuyzen van Zanten on August 9, 2023
Helicobacter pylori (H. pylori) continues to be an important pathogen, associated with peptic ulcer disease, dyspepsia, and gastric cancer. The conventional triple combination of a PPI, clarithromycin, and either amoxicillin or metronidazole is no longer recommended because its success rates have decreased to less than 60%. The recommended first-line therapy is concomitant therapy (PPI, clarithromycin, amoxicillin, and metronidazole) and second-line therapy is bismuth-based therapy (PPI, bismuth, metronidazole, and tetracycline).
By Vinicio Delgado and Dr. Wayne Lai on July 19, 2023
Insomnia is one of the most commonly reported sleep disorders at our sleep clinic. Despite its prevalence, treating it can be challenging due to its complex and multifactorial nature. A comprehensive and personalized approach to treatment is, therefore, necessary for effective management. However, providing this level of support requires significant time and resources. Offering a self-help intervention as a complement to care can help reach patients who might not otherwise receive CBTi or refuse onsite treatment.
By Drs. Kevin Lee and Persia Pourshahnazari on May 31, 2023
While not a fundamentally dangerous condition, CSU can have a significant impact on a patient’s quality of life and can be challenging to manage. Symptoms can be prolonged and can recur even after a long symptom-free period. Escalate and taper non-sedating H1-antihistamines, encourage daily antihistamine use, and add corticosteroids or refer to an allergist if needed.
By Drs. Rohit Vijh and Jason Wong on May 17, 2023
Pregnant persons should be screened for syphilis during the first trimester (or first prenatal visit), and at delivery (or any time after week 35 for those planning home births).
By Dr. Emma Coffey on April 3, 2023
Many patients don’t know that an IUD is a highly effective option for emergency contraception. We can offer patients either the 52mg LNG-IUS (up to 5 days) or the copper IUD (up to 7 days) for EC. Both options are highly effective at preventing pregnancy (>99%).
By Drs. Kevin Lee and Persia Pourshahnazari on March 21, 2023
Despite being a fairly common problem, with an estimated prevalence of 0.5–5%, chronic spontaneous urticaria (CSU) is often a challenging condition for health-care providers to diagnose and for patients to accept as a diagnosis. A diagnosis of CSU does not equate to a diagnosis of a systemic autoimmune disease. We do not routinely recommend dietary modification for CSU. We advise patients with CSU to limit alcohol intake and to take a higher dose of antihistamines prior to receiving vaccinations.
By Drs. Clara Lu and Renée Janssen on March 7, 2023
Since the publication of the 2020 ATS Clinical Practice Guideline on pharmacologic treatment in tobacco-dependent adults, I now explain the goals of pharmacotherapy for tobacco use disorder in terms of reducing the compulsion to smoke and increasing readiness to quit, rather than abstinence alone. If patients are open to the conversation, I will discuss and offer all pharmacotherapy options — but emphasize the efficacy and safety of varenicline as my preferred first-line agent.
By Dr. John van Bockxmeer, Dr. Vishal Varshney, and Anthony Lau, PharmD on February 15, 2023
I incorporate this ‘NSAID ceiling’ into my prescribing practice for anti-inflammatory medications. I typically prescribe maximum doses of 400 mg oral ibuprofen TID with meals and 10 mg intramuscular ketorolac. I counsel my patients to limit their NSAID use to a 5-day window when possible and encourage other non-pharmacological and multimodal analgesia.














Recent Comments