By Drs. Jennifer Kask and Kirsten Duckitt on January 25, 2023
Preterm birth is the leading cause of perinatal morbidity and mortality in British Columbia and worldwide. We now carefully elicit any history of previous preterm birth and offer vaginal progesterone therapy for ANY history of spontaneous preterm birth. We fill in the Special Authority Request and give out the patient handout even before the patient goes to the pharmacy. We also encourage women to continue the medications until 37 weeks of gestational age.
By Dr. Karin Kausky, Dr. Tracy Monk, and Daniela Michel, MPH on January 11, 2023
Antimicrobial resistance is recognized as a top public health threat and is estimated to be directly responsible for 5,400 deaths and $1.4 billion in health care costs in Canada in 2018 which underlines the critical importance of wise prescribing of antibiotics. Every time I prescribe an antibiotic now, I check the Bugs & Drugs guidelines via PathwaysBC.ca.
By Drs. Cheryl Young and David McVea on November 2, 2022
November is Radon Action Month. There are approximately 3,000 lung cancer deaths in Canada attributable to radon exposure each year, but there is limited awareness of radon both among the public and health care providers.
By Drs. Fiona Petigara and Joanna Cheek on September 28, 2022
A large part of physician’s day is spent on mental health and wait times to see specialists can be very long. In 2022 the BC Government created “Group Medical Visit” (GMV) codes to promote physicians to deliver services to groups of patients as “an effective way of leveraging existing resources; simultaneously improving quality of care and health outcomes, increasing patient access to care and reducing costs” (BC Gov, 2022). Physicians can now refer their patients to the Group Cognitive Behavioral Therapy program via cbtskills.ca or through PathwaysBC fillable PDF and they can also train to facilitate group medical visits.
By Dr. Konia Trouton on September 12, 2022
Patient satisfaction and continuation rates are very well documented for various contraceptives in Canada. Among the combined hormonal contraceptives — the pill, patch, and ring — only 50% of people are still using them after a year, despite all efforts to improve compliance and reduce side effects. In contrast, over 80% of people are still using long-acting and reversible IUDs a year later.
By Dr. Katarina Wind on May 3, 2022
Medical school taught me that “obesity” is a cause of morbidity and mortality, and that weight loss is its cure. I recorded patients’ BMIs and counselled them on weight-loss strategies, believing that I was helping them.
By Drs. Tandi Wilkinson and Shireen Mansouri on December 7, 2021
We are hearing from many of our medical colleagues about their distress in this time of COVID-19. Many are troubled by the fact that most of the people admitted to hospitals and intensive care units are not vaccinated. Faced with yet another variant and uncertainty, we hear that our colleagues are exhausted, frustrated, and angry. Both authors, being interested in supporting physicians to thrive in their work, have been studying compassion and its role in practitioner well-being for the last few years. As looking at this issue (and other challenges of the pandemic) through the lens of compassion has been personally helpful to both of us, we wanted to share our learnings with you.
By Dr. Linda Uyeda and Dr. Ashley Miller on July 7, 2021
The ingredients needed to create a happy workplace also largely reflect the principles of secure attachment. Across all levels within organizations, if people do not feel “safe, seen, soothed, and secure” they are more likely to make errors, breach safety protocols, and struggle working together as a team.
By Sue Barlow and Carolyn Rondeau on June 3, 2021
Concussions or mild traumatic brain injury are the most common type of traumatic brain injury. It is estimated that every year in British Columbia (BC), there are approximately 14,500 visits to the emergency department and that this number is most likely an underestimate of the “true burden of concussion”.
By Dr. Ashley Miller and Dr. Linda Uyeda on May 12, 2021
As I started to understand that this pandemic would wear on, I had to figure out how to help my patients’ families and my own family navigate our way through this totally new reality. I drew on the science of attachment, resilience and healthy relationships to make a plan. (Please stay tuned for Article #3!)
By Dr. Colleen Dy, Zerlyn Lee, and Adrienne Sim on April 7, 2021
Individuals with Chronic Pelvic Pain (CPP) often experience disruptions in multiple aspects of their reproductive health care. Routine pelvic examinations often become extremely challenging due to pain.
By Dr. Susan Hollenberg on March 17, 2021
It is prudent to reduce the risks of pneumococcal illness during this time of potentially severe respiratory sequelae of COVID-19, and the newly introduced BC Care Bundle Incentive payment includes a focus on ensuring eligible people receive this vaccine.
By Dr. Linda Uyeda and Dr. Ashley Miller on March 3, 2021
(Please stay tuned for Article #2: ‘Parenting during a pandemic’. We will expand on how to nurture these secure attachments with our children.) By Dr. Linda Uyeda (biography and disclosures) and Dr. Ashley Miller (biography and disclosures) (Members of the Child and Youth Mental Health and Substance Use Community of Practice and the Working Group […]
By Dr. Jeff Harries on December 7, 2020
Editor’s note: Here is the revised article on AUD by Dr. Harries, which more prominently emphasizes the stepwise approach in the BC AUD guidelines. We appreciate the patience of our readership and special thanks to Dr. Harries for his passion and commitment to treating AUD. We would also like to thank Dr. Keith Ahamad (co-chair […]
By Dr. Simon Moore on November 4, 2020
A 2019 systematic review of 26 studies (4 from Canada) concluded that there is a “unanimous lack of self-perceived knowledge” among practitioners regarding medicinal cannabis use. Now, when a patient asks me about cannabis, I no longer suffer from dizziness, dry mouth, and paranoia.
By Dr. Eileen Murray on October 14, 2020
Acne vulgaris is a distressing disease beginning at puberty, involving the pilosebaceous follicles of the skin on the face, chest, and back. The incidence of acne in teenagers is nearly 100%. Treating teenagers with acne was an exceptionally important part of my practice.
By Drs. Philip Lee and Stefanie Falz Mclellan on September 30, 2020
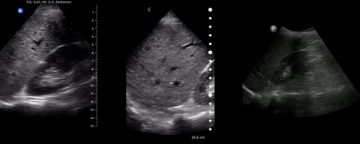
The integration of point of care ultrasound (PoCUS) in the emergency department workflow is not always easy, and these challenges have been amplified in the time of COVID-19. The COVID-19 pandemic has led to an increased interest in the use of handheld ultrasound devices as they simplify infection control procedures and take up little space in emergency rooms crowded with critical care equipment.
By Tandi Wilkinson MD CCFP-EM on April 1, 2020
I conducted a study examining effective peer support in rural Canadian physicians. (Spoiler alert: those who have had good peer support say it is essential to their career in medicine.) Here is what I am doing now to ensure I, and my team, can manage through this unprecedented time at work.
By Dr. Janet McKeown on March 11, 2020
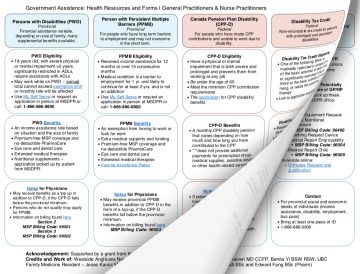
Government Assistance: Health Resources and Forms tool has helped me understand assistance with a more organized approach. It has helped me access information quickly and it has helped me be more knowledgeable about billing provincially, federally and privately. It is also an efficient tool to use in a teaching environment to help learners better understand government assistance.
By Dr. Susan Woolhouse on February 26, 2020
My past experiences during my palliative care rotations reassured me that children could benefit from bearing witness to a loved one’s death. Why would MAID be any different? I set out to learn more about how children grieve and ways in which I could support children through the dying of a loved one seeking MAID.
By Dr. Mary V. Seeman on February 5, 2020
Fellow psychiatrists often ask whether their patients with schizophrenia are aging prematurely. They point to the fact that several of their patients seem slowed down, forgetful, fidgety, and that they garble their words and stutter. These are, of course, all side effects of antipsychotic medication.
By Dr. Breay Paty on January 21, 2020
The therapeutic use of testosterone has increased dramatically in the last two decades. The reasons for this appear to be increased frequency of testing and marketing of testosterone replacement for middle-aged and older men. While men with unequivocally low testosterone levels usually benefit from hormone replacement, the risk/benefit ratio for men with equivocal (“borderline”) levels is not clear, especially men who desire fertility.
By Dr. Dan Bilsker on January 8, 2020
It is well-known that men die on average 3-4 years before women – but why? We identified three main factors contributing to Years of Life Lost by men compared to women: cardiovascular disease, suicide, and motor vehicle accidents. As a psychologist, I was intrigued by the substantial contribution of suicide.
By Dr. Lisa Nakajima on December 4, 2019
One of the risks of IUD insertion includes perforation of the uterus. Although uterine perforation is relatively uncommon and often does not cause long-term harm, it does increase the risk of unplanned pregnancy and often requires surgery. I have chosen to use endometrial aspirators that are commonly used for endometrial biopsy sampling as a sound for IUD insertions, instead of the traditional metal sounds.
By Dr. Eileen Murray on October 16, 2019
Topical corticosteroids are the most frequently used topical medications for treating skin diseases. They are cheap, extremely efficacious and almost completely free of side effects when used appropriately.
By Dr. Alisa Lipson on September 25, 2019
Now in 2019, we are learning that the incidence in girls is higher than previously thought. The girls are catching up to the boys. What is that about? Turns out that the girls are better at hiding their disability but it is there. So, we have to look harder.
By Dr. Amin Javer on September 11, 2019
Sinusitis is a commonly encountered condition for the Canadian family physician. Chronic sinusitis has worse quality of life scores than COPD, CHF or angina. The total cost of diagnosing and treating sinusitis remains one of the most expensive chronic disorders experienced by the North American population and continues to increase yearly.
By Dr. Tahmeena Ali on August 21, 2019
I now ask all patients, young and old, new to my practice and established for years, male and female, to complete an ACEs questionnaire in my clinic. I garner a new level of respect for my patients’ resilience and for the ongoing turmoil many of my young patients face. I make finding supports for these young vulnerable patients one of my top priorities—as important as a referral to a specialist or for diagnostic imaging.
By Dr. Miguel Imperial on July 30, 2019
Once I diagnose a patient with CLM based on a compatible travel history and characteristic serpiginous rash, I continue to treat the itch and inflammatory symptoms symptomatically if indicated, but I am able to much more readily offer systemic therapy with ivermectin since it no longer requires a Health Canada Special Access application.
















Recent Comments