By: Douglas Cave MSW, RSW, PhD, RPsych, MA, AMP, MCFP (Biography & Disclosures), no disclosures
What I did before:
I was frustrated at times that the students and residents did not always follow the instructions I gave. Their work was sometimes incomplete, off topic, or plainly wrong. While this was not true for most students, it was consistently true for a few each year. Teaching about empathy for example, I would invite residents to practice doing an interview with each other using empathic reflections and they would do it incorrectly. Even though I would instruct about exactly how to use empathy in an interview, they would miss most of the opportunities I thought I very clearly indentified.
While teaching the Interpersonal Gap (Chinmaya & Vargo, 2012; Wallen, 1967) as something important in clinical care to my students one year, I had the insight that the model is also true in the teaching environment. I realised that while I was giving instructions to my students, I was developing an interpersonal gap between them and me. I was speaking in ways that did not take into account the individual experience of my students. I also failed to give my instructions in a way that acknowledged that each person is different.
What changed my teaching practice:
In his conceptualization of interpersonal relationships, John Wallen identified three basic human conditions:
- Individual experience is private
- Each person is different
- People are interdependent social beings.
A lack of awareness and responsiveness to these conditions produce an interpersonal gap between people.
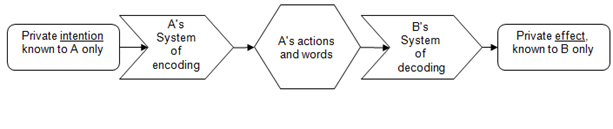
The model he developed includes the following graphic representation (Chinmaya & Vargo, 2012; Wallen, 1967), which illustrates the many factors that can influence the intention of the communicator, and the impact on the listener.
Wallen identified four communication skills to help bridge this interpersonal gap. The four communication skills are:
- Paraphrasing
- Behaviour description
- Description of feelings
- Perception checking
What I do now:
This model has changed the way I teach in that I am increasingly mindful of the possible effects of what I communicate on the residents and students. I work to be aware of my context and the context of the students while I’m encoding my communication to them. For example, since I differ from my students in life and clinical experience, generation, academic training, gender and both ethno and social culture, I am mindful of working to encode the material I teach in a way that may be more easily decoded by them. I work to match how I speak to their level of education, and any other apparent contextual features. I avoid using a reference to something that is too personal, a jargon or colloquial term that is open for interpretation and therefore not understandable to them. I use as much behavioural language as possible. I see myself giving the message to the students in a couple of different ways in the hopes that more students will be able to accurately decode the teaching material. For example, regarding the teaching of empathy, I do the following:
- Paraphrase: As an example of the use of empathy, I paraphrase back to the residents something they said earlier that same day and use empathy in my paraphrase;
- Behaviour description: Give a clear behavioural description of when they should use empathy in an interview, such as using an empathic reflection with a patient before switching topics or asking another question;
- Description of feeling: Help the residents identify what they will feel and how their patient will express their feelings when empathy is expressed accurately;
- Perception checking: In a classroom setting, I ask if there are any questions for clarification, but in a 1-1 clinical setting, I can ask the resident to explain back to me what they understand. While perception checking slows the process, it is clear that if they misunderstand and misperform the activity, the process is slowed even more when I need to explain again to have them perform the activity again.
With an awareness of how I have to work hard to ensure I encode my communication in a way that can be decoded by the students, I recognise that I work to understand their context. By understanding the students’ context, I frame my communication in a way that hopefully has the desired effect on them. I find myself asking them to explain back to me what it is they understand me to be saying (perception checking).
From the model, I recognise that the intent of what I say does not always equal the effect on the listener. Therefore, I am careful about how I build rapport with my students. I differentiate between being liked and being respected. Therefore, I am judicious in my use of self-disclosure or humour. I use self-disclosure sparingly and only general humour. I strive to develop a strong rapport with my students by developing agreements of how we are going to work together. From the model, I recognise that communication is open to interpretation and my goal is to minimise misunderstandings and increase the safety in the teaching environment. Therefore, expectations are clarified by me asking what the student wants from the learning environment and me telling the student what I expect of them in the learning environment. Perception checking is done at the end to ensure we are aligned.
To help me achieve the desired effect of my communication during teaching, I now work to ensure that I use many concrete examples such as clear clinical examples. When giving the students feedback, I work to use as much behavioural description as possible so as to minimise any sense of unintended judgement or impact. I also work to have the time and patience to hear back from the students regarding what they understand me to be saying. I have recognised that if I rush or omit the last part of hearing back from the students, I become more frustrated because it means sometimes I have to repeat the instructions after they performed the action in a different way than I expected.
References and/or Additional reading
Since John Wallen provided workshops more so than publish, the most complete description of his work can be found in:
Chinmaya, A., & Vargo, J. (2012). Improving Communication: The Ideas of John Wallen. Canadian Journal Of Counselling And Psychotherapy / Revue Canadienne De Counseling Et De PsychothéRapie, 13(3). Retrieved from http://cjc-rcc.ucalgary.ca/cjc/index.php/rcc/article/view/1947
Wallen, J. (1967). The Interpersonal Gap. Mimeographed paper, Portland, Oregon.

Recent Comments