By Dr. Eileen Murray MD FRCPC (biography and disclosures) Disclosures: Served as a consultant for the pharmaceutical industry and participated in clinical research evaluating new therapies for psoriasis and atopic dermatitis. Mitigating potential bias: Treatments or recommendations are unrelated to products/services/treatments involved in disclosure statements.
What care gaps or frequently asked questions I have noticed
Topical corticosteroids are the most frequently used topical medications for treating skin diseases. They are cheap, extremely efficacious and almost completely free of side effects when used appropriately. There are however some frequent concerns that I see:
- Patients being treated with a corticosteroid of a potency which is either too weak or too strong (one being the most potent and seven the least). Table 2
- Fear of side effects preventing optimal use.
- Patients treated with a topical corticosteroid in a less effective vehicle.
- Patients being switched to oral corticosteroids before treating with a more potent topical corticosteroid.
- Patients with undiagnosed bacterial or fungal infections being treated with topical corticosteroids.
- Patients given inadequate instructions or not followed up frequently enough.
Example comments from patients: “My doctor told me this was strong medication and I was afraid to keep using it, so I stopped after a week.” “I’m afraid it will thin my skin.” “When I stop applying the cream, the rash and itching come back. I apply it every day to prevent the rash from coming back.”
So, what do we do when our patient’s rash is not improving and how do we prevent side effects and adrenal suppression?
Data that answers these questions or gaps
Possible causes of treatment failure include the following:
- Ineffective corticosteroid molecule
- Inappropriate vehicle
- Noncompliance often from fear of side effects
- An incorrect diagnosis
Check Appendix 1: Vehicles. The effectiveness of a topical corticosteroid is equally dependent upon the potency of the corticosteroid molecule and the type of vehicle used to transport the drug into the skin. An ointment is the most effective vehicle especially on dry skin. Creams spread more easily are more cosmetically acceptable.
Check Table 1 (The site on the body affects percutaneous absorption) and Table 2 (Potency rankings of some of the commonly used topical corticosteroids) for help in deciding which corticosteroid molecule to use on a particular area. It is best to start treatment with a more potent corticosteroid rather than a mild less effective one. As the disease becomes less severe, you may reduce the potency of the steroid molecule. The more acute and severe, the more potent the drug should be.
![]() Download PDF of Appendix 1, Table 1, and Table 2.
Download PDF of Appendix 1, Table 1, and Table 2.
Because topical corticosteroids are applied directly onto the diseased skin, efficacy is enhanced, and the risk of systemic side effects is markedly reduced. An example of this are patients with systemic lupus who have discoid skin lesions. Although they receive systemic steroids for their disease, the discoid skin lesions will often only resolve with addition of a potent topical corticosteroid.
It is also safer to use potent or super potent topical corticosteroids even over a large area than using the systemic drug. This is because skin cells metabolize corticosteroid before it can be absorbed, meaning the amount of active drug entering the circulation is much less than the amount applied. This reduces the risk of adrenal suppression.
Also, normal skin is a better barrier and metabolizes more drug than diseased skin, so as the skin disease improves, absorption is decreased substantially – a built in safety net! An example of this was a sixteen-year-old girl with widespread striae over her arms and legs as a result of applying clobetesol propionate cream daily for two years to prevent her eczema from recurring. Her adrenal function remained normal.
Adrenal suppression can occur when large areas of the body are treated with potent topical corticosteroids. Children have a larger surface area to weight ratio allowing more absorption compared to adults. However, once the medication is discontinued recovery is rapid.10 Mild to moderately potent topicals almost never suppress adrenal function. Growth retardation has been reported in children with atopic dermatitis. It seems to be temporary and reversible.4
What I recommend (practice tips)
Prescribe the correct amount needed to cover the surface area once or twice a day until the next appointment and control the number of repeats. Explain to your patient to apply just a small amount and rub it gently into the skin until it disappears. The more effective the medication, the less time needed for healing. Using a more potent topical corticosteroid will reduce the likelihood that the patient will require systemic corticosteroids. It also reduces the need for chronic treatment and makes it more likely that the patient will use it only when needed.
Instruct patients to apply super potent to moderately potent (ranks 1-4) preparations once daily and potent to low potency (ranks 5, 6 and 7) preparations twice daily. Many of the new corticosteroid molecules, such as prednicarbate and mometasone propionate, accumulate in the skin producing a reservoir so that they need only be applied once a day.
Intermittent use also reduces the amount of corticosteroid required to control the disease.7,8,11 In a study involving 174 children with mild to moderate atopic dermatitis followed for 4 ½ months:
- group 1 was treated with 1% hydrocortisone cream twice daily for 7 days, and
- group 2 was treated with 0.1% betamethasone valerate ointment twice daily for 3 days.
No differences were found between the two groups in either efficacy or safety.
Reassess your patient’s response. It is important to reassess your patient’s response for three reasons:
- Many patient’s fear possible side effects especially thinning of the skin.
They need reassurance. Do not alarm your patients unnecessarily, rather explain to them carefully and optimistically how to use the medication. It has been shown that a parent’s compliance in using topical corticosteroids on their children’s skin is almost completely dependent upon their confidence and trust in you, their doctor.1,3 - Incorrect diagnosis.
If your patient has not improved or particularly if the rash has spread or become worse, reconsider your diagnosis. Both fungal and bacterial infections are made worse when treated with topical corticosteroids. A scaly rash on the scalp treated for a month with topical corticosteroids was not psoriasis but impetigo with crusting. A facial rash diagnosed as eczema that spread with a red center and marked scaling at the edges was a tinea infection. - Patients who keep using the medication for fear the rash will recur.
This is a particular problem for patients with chronic disease. To reduce the incidence of local side effects, instruct your patients to stop applying the corticosteroid when the skin disease has cleared. However, you have to explain when that is. Be explicit. When the skin is smooth and no longer itchy, they can stop applying the medication. Post inflammatory hyper or hypopigmentation and/or residual erythema are expected, do not require treatment and slowly resolve. Explain to patients with chronic disease that the medication loses its efficacy with chronic use. Also explain that the drug works by returning diseased skin to its normal thickness (diseased skin is puffy and thick) and that if they continue to use it when the disease is gone, the normal skin will become thinner.
Use nonsteroidal creams to help prevent recurrences. Treating dry skin with daily moisturizers is extremely beneficial. One of the side effects of corticosteroids is that they dry the skin. It’s best to always have your patients apply a moisturizer daily. If they do, they will require less corticosteroid.
Minimize topical side effects:
- Acne and perioral dermatitis: exacerbation of pre-existing acne and the initiation of perioral dermatitis are the most common local side effects. Warn patients with hand dermatitis not to touch their face after applying their medication. Perioral dermatitis occurs mainly because a more potent corticosteroid then necessary has been used to treat a facial dermatitis. The patients develop a rebound flare when they stop the medication and therefore continue to use it. Properly timed follow-up visits and a limit on repeats is preventative.
- Skin atrophy – epidermal thinning, telangiectasia, striae and easy bruising occurs with overuse. Corticosteroids inhibit both fibroblast collagen formation and epidermal cell division. Easy bruising and telangiectasia result from the loss of the supporting collagen around the vessels. Overall, the changes induced resemble those of normal aging.
Patients who are given clear instructions, prescribed an appropriate amount and followed up to determine the response to treatment rarely develop side effects.
Resources:
![]() Download PDF of Appendix 1, Table 1, and Table 2.
Download PDF of Appendix 1, Table 1, and Table 2.
Vehicles:
The vehicle makes up 95 to 99.9% of a topical medication. The main vehicles are ointments, creams, lotions, gels, and pastes. It is important to choose the correct vehicle.
- An Ointment (water in oil emulsions) allows the best penetration of the active ingredient and is best for dry, sensitive skin, and especially for thick plaques. They are also most effective for disease on thick skin such as the palms and soles.
- Creams (oil in water emulsions) are less greasy, spread more easily and are better tolerated. They may sting upon application and do not hydrate the skin as well as ointments
- Lotions (oil or powder in water emulsions) are best for treating large areas. They may cause stinging and dryness. Combinations of anti-itch ingredients along with a corticosteroid in a lotion are helpful for treating widespread itching as can occur with a drug rash.
- Gels (mixtures of water, alcohol or acetone) are best for oily or hairy skin.
- Pastes (powder in an ointment) are very useful for wet intertriginous areas. The powder absorbs moisture and the ointment lubricates and soothes the skin. Diaper creams are a good example.
Table 1: The site on the body affects percutaneous absorption
| Site | Percutaneous absorption | Best vehicle | Local factors influencing absorption |
| Palms | 0.83 X | Ointment | thick stratum corneum |
| Soles | 0.14 X | Ointment | thick stratum corneum |
| Extremities (flexural surface) | 1.0 X | Ointment for dry skin, Cream | Index |
| Extremities (extensor surface) | 3.6 X | Ointment for dry skin, Cream or Lotion | Skin thinner from chronic sun exposure |
| Intertriginous Areas | 3.6 X | Cream, Lotion, Paste | Self Occlusion and Increased moisture |
| Face | 6 – 13 X | Cream, Lotion, Gel | Highly vascularized and numerous follicular openings |
| Scrotum | 42 X | Cream, Lotion | Increased moisture, self occlusion |
| Eyelids | 42 X | Ointment | Thin skin |
Table 2: Potency Rankings of some of the commonly used topical corticosteroids
| Corticosteroids molecule | Vehicle | Potency Rank Most to least | Daily application frequency | When to use |
| clobetasol propionate .05% | cream or ointment | 1 | OD | Palms and soles severely lichenified plaques |
| Betamethasone Dipropionate .05 % | Cream or ointment | 1 | OD | Plaques, Severe acute inflammation |
|
Amcinonide 0.1% OD |
Ointment | 2 | OD | Thick Scaly Plaques, Dry lichenified Plaques of chronic eczematous rashes |
| Mometasone Furoate 0.1% | Ointment | 2 | OD | |
| Betamethasone Valerate 0.1% | Ointment | 3 | OD or BID | |
|
Amcinonide 0.1%
|
Cream | 3 | BID | Acute inflammation |
| Hydrocortisone 17 valerate 0.2% | Ointment | 4 | BID | Moderately severe chronic or subacute eczemaatous rashes |
| Triamcinolone acetonide 0.1% | Ointment | 4 | BID | |
| Mometasone Furoate 0.1% | Cream or lotion | 4 | OD | |
| Betamethasone valerate 0.1% | Cream | 5 | BID | Mild or moderately severe acute eczematous rashes |
| Hydrocortisone 17-Valerate 0.2% | Cream | 5 | BID | |
| Triamcinolone Acetonide 0.1% | Cream | 5 | BID | |
| Betamethasone Valerate 0.05% | Lotion | 6 | BID | Scalp |
| Desonide 0.05% | Cream or ointment | 6 | BID or TID | Chronic eczematous rashes on thin or vascularized skin |
| Hydrocortisone 1% | Cream or ointment | 7 | BID or TID |
Photos:
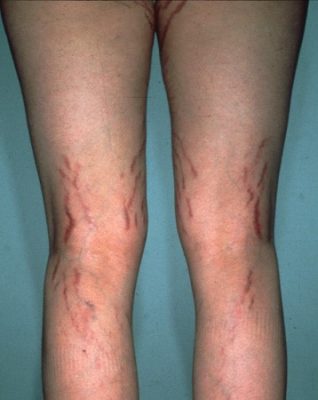
Striae resulting from the application of clobetasol propionate cream daily for two years.
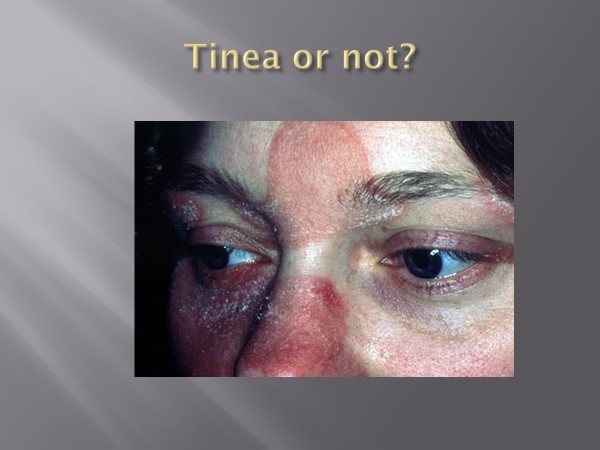
Tinea incognito of the face. Scaly edges are not seen in an eczematous rash.
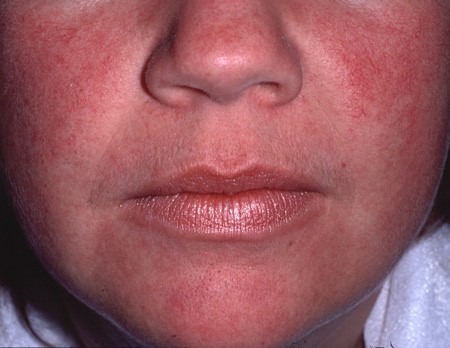
Facial telangiectasia from over ten years daily application of fluocinolone acetonide.
References:
- Charman CR, Morris AD, Williams HC. Topical corticosteroid phobia in patients with atopic eczema. Br J Dermatol. 2000;142(5):931-936. DOI: 10.1046/j.1365-2133.2000.03473.x. (Request with CPSBC or view with UBC)
- Drake LA, Dinehart SM, Farmer ER et al. Guidelines of care for the use of topical glucocorticosteroids. J Am Acad Dermatol. 1996;35(4):615-619. DOI: 10.1016/S0190-9622(96)90690-8. (Request with CPSBC or view with UBC)
- Fukaya M. Why do patients with atopic dermatitis refuse to apply topical corticosteroids? Dermatology. 2000;201(3):242-245. DOI: 10.1159/000018495. (Request with CPSBC or view with UBC)
- Patel L, Clayton PE, Jenney ME, Ferguson JE, David TJ. Adult height in patients with childhood onset atopic dermatitis. Arch Dis Child. 1997;76 (6):505-508. DOI: 10.1136/adc.76.6.505. (View)
- Raimer SS. The safe use of topical corticosteroids in children. Pediatric Annals. 2001;30(4):225-229. DOI: 10.3928/0090-4481-20010401-12. (Request with CPSBC or view with UBC)
- Reitamo S, Remitz A, Kyllonen H, Saarikko J, Granlund H. Topical noncorticosteroid immunomodulation in the treatment of atopic dermatitis. Am J Clin Dermatol. 2002;3(6):381-388. DOI: 10.2165/00128071-200203060-00002. (View with CPSBC or UBC)
- Veien NK, Olholm Larsen P, Thestrup-Pedersen K, Schou G. Long-term intermittent treatment of chronic hand eczema with mometasone furoate. Br J Dermatology. 1999;140(5):882-886. DOI: 10.1046/j.1365-2133.1999.02819.x. (Request with CPSBC or view with UBC)
- Lagos BR, Maibach HI. Frequency of application of topical corticosteroids: an overview. Br J Dermatol. 1998;139(5):763-766. DOI: 10.1046/j.1365-2133.1998.02498.x. (Request with CPSBC or view with UBC)
- Maibach HI, Stoughton RB. Topical corticosteroids. Med Clin North Am. 1973;57(6):1253-1264. (Request with CPSBC or UBC)
- Patel L, Clayton PE, Addison GM, Price DA, David TJ. Adrenal function following topical steroid treatment in children with atopic dermatitis. Br J Dermatol. 1995;132(6):950-955. DOI: 10.1111/j.1365-2133.1995.tb16954.x. (Request with CPSBC or view with UBC)
- Thomas KS, Armstrong S, Avory A, et al. Randomised controlled trial of short bursts of a potent topical corticosteroid versus prolonged use of a mild preparation for children with mild or moderate atopic eczema. Br J Dermatol. 2002;324(7340):768. DOI: 10.1136/bmj.324.7340.768. (View)

Dear Dr. Murray
this is a BRILLIANT resource
I would like to seek your permission to reference / provide these materials as appendices in undergrad med
grateful if you would let me know your thoughts on this
thank you very much !
Great article, thank you
Can you provide some examples of the typical amounts/volumes you prescribe for standard areas of the body?
I generally advise dermatitis patients that, if told by a pharmacist to use the med “sparingly”, follow MY advice, not to be stingy.
“How much topical medication do you need to prescribe for your patient?” is a very good question.
The medication should be rubbed gently onto the affected area until it is absorbed by the skin. A small amount goes a long way.
About 30grams of an ointment or cream will cover the total body surface.
To help you decide you can follow the “finger tip unit” rule.
One FTU is the amount of topical medication spanning the ventral tip of the index finger to the distal skin crease from a tube with a 5mm nozzle.
That amount is about 1/2 gram and will cover the equivalent area of two adult hands lying flat on the skin.
That amount applied twice a day for two weeks would require a 15 gram tube.
One of the dermatologists who did some resident teaching for us (Dr. Lewis in Kamloops) had a good, easily explained way of describing to patients how much cream should cover how much skin: the rice-to-toonie ratio. An amount of cream the size of a grain of rice should cover an area of skin the size of a toonie.
Excellent review of use of topical steroids. Thank you.
HSV-1 and HSV-2. Both virus types can cause sores around the mouth (herpes labialis) and on the genitals (genital herpes). It’s also crucial to learn as much as you can about your diagnosis. Seek options, Find out about what’s out there that could help, ( worldrehabilitateclinic com
Why does the TABLE 2 say to use more than once a day for ranks 1-4?
Earlier in the arrticle you say, “Instruct patients to apply super potent to moderately potent (ranks 1-4) preparations once daily…….Many of the new corticosteroid molecules, such as prednicarbate and mometasone propionate, accumulate in the skin producing a reservoir so that they need only be applied once a day.”
Thank you for your paper.